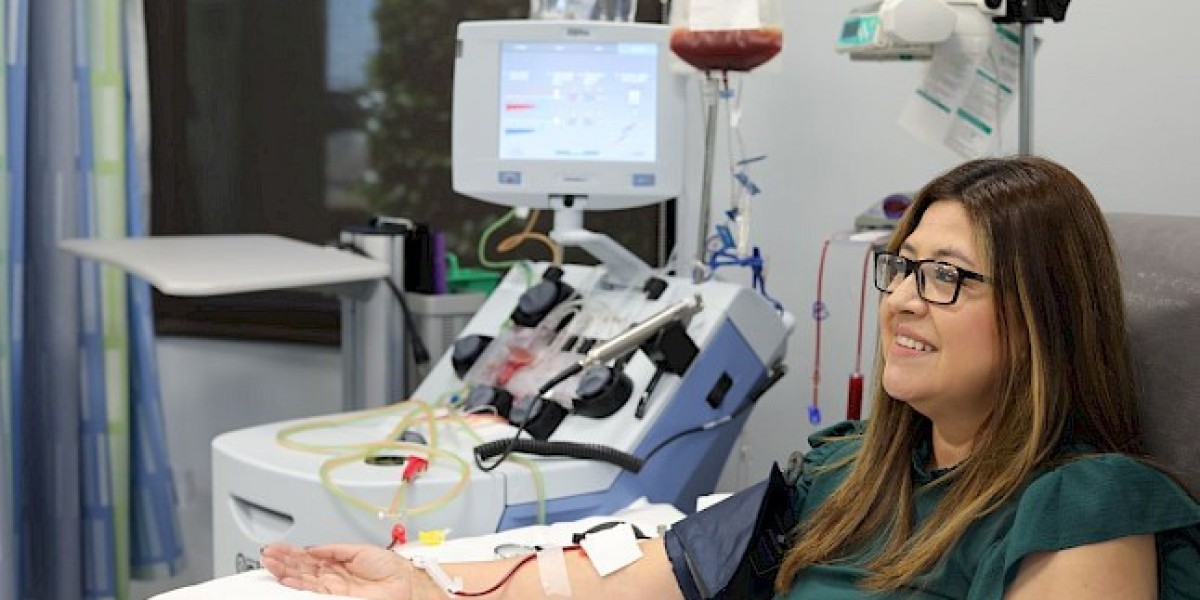
In a crowded hospital transfusion unit, machines rarely pause, but people do. A quiet shift in demand patterns, supply constraints, and evolving clinical protocols has begun to reshape how clinicians think about blood component separation. These changes are not subtle anymore, they are being felt as apheresis market disruptions that affect procurement decisions, treatment planning, and even patient prioritization in critical care settings.
What was once a predictable clinical support function is now under pressure from rising case complexity and expanding indications. Across tertiary hospitals and specialty centers, teams are adjusting workflows to manage sudden variability in demand, especially where precision-based blood processing is essential. This evolving instability is redefining expectations for both clinicians and device manufacturers.
Apheresis Market Structural Shifts Driven By Clinical Dependency And Technology Evolution
The apheresis market is undergoing a structural transformation as healthcare systems increasingly rely on targeted blood component separation for treating autoimmune disorders, hematologic conditions, and transplant support. What was once a niche intervention is now embedded into mainstream treatment pathways, especially in critical care units where rapid intervention is required.
A key driver behind this shift is the rising awareness of apheresis procedure applications in both emergency and planned therapeutic settings. Hospitals are expanding capacity, but demand is growing faster than infrastructure upgrades, creating operational bottlenecks. Procurement teams are now reassessing vendor reliability, machine scalability, and consumable availability as core decision-making factors rather than secondary considerations.
In parallel, the expansion of outpatient care models is changing utilization patterns. Instead of centralized inpatient dependency, more patients are undergoing repeated sessions across outpatient cycles. This shift has added unpredictability to scheduling systems, forcing administrators to rethink capacity planning and resource allocation strategies.
At the same time, the interpretation of apheresis meaning has also evolved within clinical circles. It is no longer seen merely as a technical blood separation method but as a precision therapy platform integrated into disease management protocols. This reframing has elevated its strategic importance in hospital planning committees and specialty care departments.
Therapeutic Apheresis Adoption Trends Reshaping Hospital Treatment Protocols
Within the broader therapeutic landscape, therapeutic apheresis is emerging as a cornerstone for managing complex immune-mediated and neurological conditions. Its growing adoption is being fueled by clinical evidence supporting improved outcomes in conditions that previously relied on limited pharmacological options.
However, this growth is not without friction. Hospitals are reporting uneven access to trained operators, fluctuating supply of disposable kits, and variability in machine performance across different apheresis types. These inconsistencies are contributing to delays in treatment initiation and creating pressure on clinical scheduling systems.
Another layer of disruption comes from evolving reimbursement frameworks. As payers reassess coverage models for advanced procedures, hospital administrators must balance cost containment with clinical necessity. This tension is influencing adoption curves, particularly in mid-sized healthcare facilities that lack dedicated apheresis units.
Training and workforce readiness are also becoming critical constraints. The complexity of modern apheresis systems requires specialized training, yet staffing pipelines are not expanding at the same pace as procedural demand. As a result, experienced operators are increasingly centralized in high-volume centers, leaving smaller facilities dependent on rotational expertise.
Technology innovation, while promising, is also introducing transitional challenges. New-generation devices offer improved automation and safety features, but integration into legacy hospital systems often requires workflow redesign. This creates temporary inefficiencies that contribute further to operational strain.
Across the industry, stakeholders are also reevaluating data-driven decision-making. Real-time monitoring of utilization patterns is helping hospitals identify inefficiencies, but the lack of standardized reporting across platforms limits full-scale optimization. This fragmentation continues to amplify pressure on system-wide coordination.
Despite these challenges, the long-term trajectory remains expansionary. The increasing reliance on apheresis procedure in multidisciplinary care settings suggests sustained growth, particularly as personalized medicine continues to influence treatment design. What is changing is not the relevance of the technology, but the complexity of delivering it efficiently at scale.
Looking forward, resilience in this sector will depend on how quickly stakeholders can align clinical demand with operational capacity. Hospitals that invest in integrated planning, workforce training, and adaptable infrastructure are likely to navigate current pressures more effectively than those relying on legacy systems.
The apheresis landscape is no longer defined by isolated clinical use cases but by interconnected systems of care delivery, supply chain responsiveness, and technological adaptation. As these forces continue to evolve, the market will reward agility over scale, and precision over volume. What emerges next will not simply be growth, but a redefinition of how therapeutic separation technologies are embedded into modern medicine.